Peri-implant mucositis, frequently encountered in dental health discussions, is an increasingly relevant topic in the era of advanced dental restorations. This condition, characterized by inflammation of the soft tissues surrounding dental implants, presents both a challenge and a learning opportunity for patients and dental professionals.
As we delve into the nuances of this condition, we aim to unravel its causes, identify its symptoms, and explore the most effective strategies for prevention and management. This exploration is pivotal for those with dental implants and enlightening for anyone invested in maintaining optimal oral health.
What are Peri-implant Mucositis lesions?
Peri-implant mucositis lesions manifest as inflammatory conditions impacting the soft tissues encircling a dental implant. Noted for symptoms such as redness, swelling, and bleeding upon probing, these lesions do not entail the loss of supporting bone structure surrounding the implant. Typically induced by the accumulation of bacterial plaque, these lesions often perceived as an initial stage of peri-implant disease, akin to gingivitis around natural teeth.
If not addressed promptly, it can advance to peri-implantitis, a more severe condition involving bone loss that can jeopardize the implant’s stability. Early detection and intervention play a pivotal role in effectively managing and ensuring the enduring health of dental implants.
What Causes Peri-implant Mucositis
Peri-implant mucositis, a common yet concerning condition in dental implant care, is often triggered by specific factors that compromise the health of the tissues surrounding dental implants. Understanding the causes of peri-implant mucositis is essential for prevention and effective management, ensuring the longevity and health of dental implants.
Causes of Peri-implant Mucositis:
- Poor Oral Hygiene: The primary cause of peri-implant mucositis is the buildup of bacterial plaque around the implant, similar to how plaque affects natural teeth.
- Improper Implant Placement: Implants positioned in areas difficult to clean can lead to plaque accumulation, increasing the risk of inflammation.
- Tobacco Use: Smoking is a significant risk factor, as it impairs blood flow and healing, exacerbating the inflammatory response.
- Pre-Existing Dental Conditions: Conditions like periodontitis can predispose patients to develop peri-implant mucositis due to existing bacteria and inflammation.
- Ill-Fitting Dental Prostheses: Prosthetics that do not fit properly can trap food and bacteria, leading to increased plaque buildup.
- Diabetes and Systemic Diseases: Patients with uncontrolled diabetes or other systemic conditions that affect the immune response are more susceptible to infections, including peri-implant mucositis.
- Genetic Factors: Individual genetic predisposition can affect the susceptibility to and severity of peri-implant mucositis.
- Mechanical Overload: Excessive force on the implant from teeth grinding (bruxism) or misaligned bite can contribute to tissue inflammation.
Recognizing and tackling the root causes is a fundamental measure for sustaining the health of dental implants. Consistent dental check-ups, meticulous oral hygiene practices, and addressing risk factors such as smoking and diabetes are essential preventive measures against this condition. Through a comprehensive understanding of the diverse factors contributing to peri-implant mucositis, collaboration between implant patients and dental professionals becomes instrumental in securing dental implants’ enduring success and well-being.
Signs and Symptoms of Peri-implant Mucositis

Peri-implant mucositis, a prevalent issue in dental implant care, presents specific signs and symptoms crucial for early diagnosis and management. Identifying these indicators is key for patients with dental implants to ensure timely intervention and prevent the progression to more severe peri-implant diseases.
Signs and Symptoms of Peri-implant Mucositis:
- Bleeding on Probing: Like gingivitis, bleeding during brushing or dental probing is common.
- Gum Redness and Swelling: The gum tissue around the implant appears red and swollen, indicating inflammation.
- Tenderness: The affected area may feel tender or sensitive to touch.
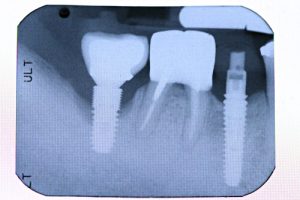
- No Bone Loss: Distinguishing it from peri-implantitis, peri-implant mucositis does not involve bone loss around the implant.
- Slight Increase in Probing Depth: When probed, a minor increase in the depth around the implant can indicate mucositis.
- Possible Suppuration: The presence of pus, although less common, may occur, signifying infection.
- Altered Gum Texture: Changes in color and texture, such as a shinier or swollen appearance of the gum tissue around the implant.
- Absence of Pain: Peri-implant mucositis often does not cause significant pain, which can delay diagnosis and treatment.
Recognizing the signs and symptoms of peri-implant mucositis is crucial for maintaining the health and longevity of dental implants. Regular dental visits and proper oral hygiene are essential in detecting and managing this condition early. Patients should monitor for changes in the implant area and consult their dentist if symptoms arise. Early intervention can effectively mitigate the impact of peri-implant mucositis, maintaining the integrity and functionality of dental implants.
Best treatment options
Effective management is critical to prevent its progression to more severe implant-related complications. Exploring the best treatment options for this condition is key to preserving the health of dental implants and the surrounding tissues.
Best Treatment Options for Peri-implant Mucositis:
- Improved Oral Hygiene: Rigorous oral hygiene practices, including brushing and flossing techniques, are fundamental in treating peri-implant mucositis.
- Professional Cleaning: Regular professional cleanings by a dentist or dental hygienist to remove plaque and calculus around the implant.
- Antimicrobial Rinses: Use antimicrobial mouth rinses, as a dentist prescribes, to reduce bacterial load in the oral cavity.
- Localized Therapy: Application of local antiseptics or antibiotics directly to the affected area.
- Mechanical Debridement: Removal of plaque and calculus from the implant surface, typically using non-abrasive instruments to avoid damaging the implant.
- Laser Therapy: In some cases, laser therapy may be employed for its anti-inflammatory and antimicrobial effects.
- Patient Education: Educating patients about the importance of maintaining implant health and the correct techniques for implant care.
- Regular Follow-Ups: Scheduled follow-up appointments with the dental professional to monitor the condition and adjust treatment as necessary.
- Modifying Risk Factors: Addressing modifiable risk factors such as smoking cessation and controlling systemic conditions like diabetes.
The successful non-surgical treatment hinges on early intervention and comprehensive care strategies. A combination of improved oral hygiene, professional dental care, oral implants, and patient education forms the cornerstone of effective management. Regular monitoring and modifications in treatment approaches, as needed, are crucial in resolving peri-implant mucositis and maintaining long-term implant health.
How to prevent Peri-implant Mucositis
Preventing peri-implant mucositis is essential for the long-term success of dental implants. By implementing proactive measures and maintaining diligent oral hygiene, patients can significantly reduce the risk of developing this inflammatory condition and ensure the longevity of their dental implants.
Prevention Strategies for Peri-implant Mucositis:
- Maintain Optimal Oral Hygiene: Regular and thorough brushing and flossing to remove plaque and prevent bacterial accumulation around implants.
- Routine Dental Check-Ups: Regular visits to the dentist for professional cleanings and examinations of implants.
- Quit Smoking: Smoking cessation is crucial as it increases the risk of peri-implant diseases.
- Control Systemic Health Conditions: Managing systemic conditions like diabetes can affect gum health.
- Use of Interdental Brushes: Utilizing interdental brushes or water flossers to clean hard-to-reach areas around implants.
- Balanced Diet: Consuming a healthy diet to support overall oral health.
- Avoid Excessive Pressure on Implants: Be mindful of habits like teeth grinding, which can put undue stress on implants.
- Patient Education: Understanding the importance of implant care and maintenance for preventing peri-implant diseases.
- Immediate Addressal of Gum Inflammation: Seeking prompt dental care at the first sign of gum inflammation or discomfort.
Preventing peri-implant mucositis involves a combination of excellent oral hygiene, regular dental visits, and lifestyle modifications. By taking these proactive steps, patients can effectively safeguard their dental implants against inflammation and ensure optimal oral health. Understanding and adhering to these preventative measures is key to dental implants’ long-term success and health.
What Happens if Peri-implant Mucositis is Left Untreated
Leaving peri-implant mucositis untreated poses significant risks to dental implant health. This seemingly minor condition can escalate into more severe complications, emphasizing the need for prompt and effective management.
Consequences of Untreated Peri-implant Mucositis:
- Progression to Peri-implantitis: The most significant risk is the progression from mucositis, a soft tissue inflammation, to peri-implantitis, which includes soft tissue inflammation and bone loss around the implant.
- Implant Failure: Peri-implantitis can weaken the supporting bone, potentially resulting in implant loosening and failure.
- Increased Risk of Infection: Ongoing inflammation can lead to persistent infection, posing a local and systemic risk.
- Aesthetic Complications: The aesthetic appearance of the implant and surrounding gum tissue can be compromised, affecting the overall look of the dental restoration.
- Costly and Complex Treatment: Treating advanced peri-implant diseases often requires more complex and costly interventions than early-stage mucositis.
Prompt treatment is essential to prevent its progression to more severe dental issues. Early intervention, regular dental check-ups, and good oral hygiene are crucial in managing this condition. Addressing peri-implant mucositis early helps maintain the health and longevity of dental implants, ensuring they remain a successful and lasting solution for dental restoration.
References
Treatment of Peri-implant Mucositis: A Systematic Review
https://journals.lww.com/implantdent/fulltext/2015/02000/treatment_of_periimplant_mucositis__a_systematic.4.aspx
Biologic Complications – Post-Treatment Complications and Management
https://www.for.org/en/treat/treatment-guidelines/edentulous/aftercare/post-treatment-complications-and-management/biologic-complications
Guidance Notes for the Classification of Periodontal and Peri-Implant Diseases and Conditions
https://www.efp.org/fileadmin/uploads/efp/Documents/Campaigns/New_Classification/Guidance_Notes/report-04.pdf
Microbiological and clinical analysis of the relationship between smoking habits and peri-implant diseases
https://www.sciencedirect.com/science/article/pii/S0300571217300957





Comment here